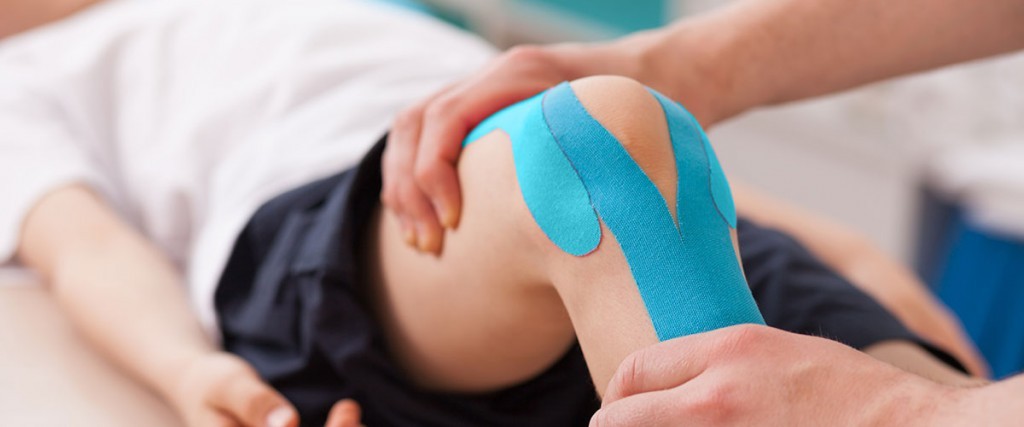
Knee disorders and pain
Many people experience knee pain as the result of either acute injury (a problem that occurs following a single event) or repetitive trauma and strain. However, in some cases—for example, in situations involving underlying degenerative conditions—the exact cause of the pain may be unknown to the person experiencing it. Knee pain can lead to difficulty or impairment with activities such as walking, standing up after sitting, and ascending or descending inclined surfaces, especially stairs.
The knee joints are subjected to many stresses in daily living. They provide crucial support to many functional activities. Due to their constant use with walking, running, standing, etc., normal wear and tear can cause pain. Injuries caused by excessive strain, twisting, or blunt force can occur. Any knee injury can cause a significant change in every day mobility. Listed are some common injuries/procedures involving the knee:
- Osteoarthritis/Degenerative Joint Disease. This is a common condition involving the knee where there is significant wear on the cushioning between the bones causing pain.
- Ligament sprain and/or strain. There are several elastic fibers called ligaments that help to stabilize the knee joint. They include the anterior cruciate ligament (ACL), the medial collateral ligament (MCL), the posterior cruciate ligament (PCL), and lateral collateral ligament (LCL). When excessive force is placed on the knee in any given direction, a sprain or tear can occur to that tissue causing pain and instability.
- Meniscus Tear. The cushioning in the joint becomes disrupted and can cause pain and a “catching” sensation. The knee may also “buckle” or “lock”.
- Patellar Dislocation/Subluxation. The patella, or knee cap, tracks poorly within its groove and can be pulled out of alignment due to poor ligament stability or muscle imbalances.
- Total Knee Replacement. The joint, bones, and connective tissue are replaced with a synthetic material to help rebuild joint structure and decrease pain.
Common problems and injuries:
- knee arthritis and DJD.
- Anterior knee pain/ Patella-femoral Maltracking / Syndrom
- patellar tendinis/tendinosis ( Jumpers knee)
- knee bursitis
- Inner knee pain
- meniscus tears non-surgical and post surgical
- ACL/PCL tears – pre, post surgery as well as non-surgical approach
- MCL tears non- surgical and post surgical
- pes anserine bursitis/tendinopathy
- medial retinacular pain syndrome
- Runners knee (patella-femoral pain syndrome)
- PFPS (patella-femoral pain syndrome in non runners)
- ITB band syndrome
Categories of Knee Pain
There are three main categories of knee pain. They are:
- Acute pain: Pain that occurs one day to one week after injury. Because this is the most severe type of knee pain, it is crucial that you rest the knee and allow it to heal before resuming activity.
- Sub-acute pain: Pain that occurs two to six weeks after injury. During this time, you can typically begin to engage in gentle motion to help promote mobility.
- Chronic pain: Pain that lasts more than two or three months. If you are experiencing chronic knee pain, you should seek medical care to identify the cause.
Locations of Knee Pain
The specific site of your knee pain can provide clues about its source. By uncovering and analyzing those clues, your physical therapist can create the most effective treatment plan possible. Here are some of the most common knee pain locations:
- Front of the knee: Pain in the front of the knee is often the result of an issue with the kneecap—namely, its position and motion. A common diagnosis related to frontal knee pain is patellofemoral stress syndrome, or PFSS. This condition involves inflammation of the kneecap and the tendon between the shin and the kneecap. Those suffering from PFSS may have trouble running, jumping, kneeling, or walking up or down stairs.
- Inside of the knee: Pain on the inside of the knee often occurs as the result of athletic injury—specifically, planting the foot and then twisting the body over it. This can lead to damage to the medial meniscus or medial collateral ligament. In the absence of injury, pain in this location may be the result of other wear and tear or chronic conditions such as arthritis.
- Outside of the knee: Pain on the outside of the knee can result from damage to any number of structures, including various ligaments and tendons (especially the hamstring tendon that runs through this area). Additionally, stress to the iliotibial band (a.k.a. IT band) often causes pain in this region. The IT band is a thick piece of tissue that goes from the outer hip to the front of the knee. Sometimes, the IT band becomes inflamed at the point where it crosses the knee, producing a burning sensation whenever the knee bends. This condition, known as IT band syndrome, usually results from overuse and is common in endurance athletes.
- Back of the knee: Pain behind the knee usually results from hamstring tightness or trauma, but in rare instances, it may indicate a Baker’s cyst, which is an abnormal swelling of the back of the knee joint.
Treatment for Knee Pain
If you suffer an acute injury to the knee, it’s time for RICE—rest, ice, compression, and elevation—and fast! The pain and inflammation should subside enough to resume gentle motion within a few days. If the pain persists for more than two or three weeks, you should seek professional physical therapy services.
At iMOVE, we can evaluate your pain and provide you with the appropriate diagnosis and a personalized treatment plan. When you first begin physical therapy, We will conduct a variety of tests and assessments to gain as much knowledge as possible about your specific knee condition. These include:
- Gait analysis: By observing and assessing the motions you go through as you walk or run, your PT can identify subtle deviations or abnormalities that may point to a larger problem.
- Palpation: we may feel around your knee to determine whether any anatomical abnormalities are at play. He or she also may test different areas of the knee to see where the pain is most intense.
- Range of motion tests: Range of motion (or ROM) refers to how far you are able to bend or extend your leg at the knee joint. ROM measurements give us insight into the degree and location of your knee injury.
- Strength tests: Muscle imbalances or weaknesses are often to blame for knee issues, and strength assessments help us determine whether those factors exist in your case. That way, we can weave appropriate strength-building exercises into your treatment plan.
- Girth and swelling measurements: The amount of swelling present in your knee joint may affect the type of, and timeline for, therapy treatment that the PT recommends.
- Special tests: There are numerous special tests intended to determine exactly which knee structures are causing your knee pain. By performing these tests, we can pinpoint the source of the pain and gain a better understanding of what is causing the problem.
After completing the necessary tests, we will formulate a rehabilitation program—often referred to as a plan of care—to rehabilitate your injury and alleviate your pain. This plan will involve a variety of exercises designed to improve strength, mobility, and flexibility as well as correct any deficiencies noted in these areas. These may include:
- Walking (progressively increasing pace)
- Water aerobics
- Swimming
- Cross-training (e.g., using a cross-country ski machine)
- Using a soft-platform treadmill
Your plan of care will most likely include a home exercise program, which is a set of exercises you must complete at home at intervals specified by your PT. Additionally, we may use ultrasound, hot-cold therapy, and other passive treatment methods to relieve pain, increase blood flow, and stimulate muscles. In many instances, manual therapy (hands-on manipulation, mobilization, or massage) may be appropriate. we also may recommend that you use a supportive device—such as a cane or brace—to take pressure off of your knee as it heals.
While the frequency and duration of your therapy sessions will depend on the type and extent of your injury, you should expect to attend therapy two to three times per week for approximately three to six weeks. It is absolutely crucial that you follow the plan given to you as closely as you can. That way, you will regain normal mobility—and eliminate your knee pain—as quickly as possible.